Sebaceous Carcinoma: Symptoms, Causes, Diagnosis, Treatment & Survival Rates
~Introduction
Sebaceous carcinoma is a rare but aggressive malignant tumor that arises from the sebaceous glands — the oil-producing glands in the skin. Although uncommon, this cancer can be life-threatening if not detected early. It most frequently affects the eyelids but can occur anywhere on the body where sebaceous glands are present.
Because sebaceous carcinoma often mimics benign skin conditions such as chalazion or blepharitis, delayed diagnosis is common. Early recognition, prompt biopsy, and appropriate treatment significantly improve outcomes.
This comprehensive article covers sebaceous carcinoma symptoms, causes, risk factors, diagnosis, staging, treatment options, survival rates, recurrence, and prevention strategies.
~What Is Sebaceous Carcinoma?
Sebaceous carcinoma is a malignant tumor that originates from sebaceous glands. These glands are responsible for secreting sebum, an oily substance that lubricates skin and hair.
There are two main types:
Ocular Sebaceous Carcinoma – Occurs in the eyelid (most common form)
Extraocular Sebaceous Carcinoma – Occurs on other areas such as the head, neck, trunk, or genital region
Ocular sebaceous carcinoma accounts for approximately 75% of cases.
~Where Does Sebaceous Carcinoma Occur?
1. Eyelid (Most Common Location)
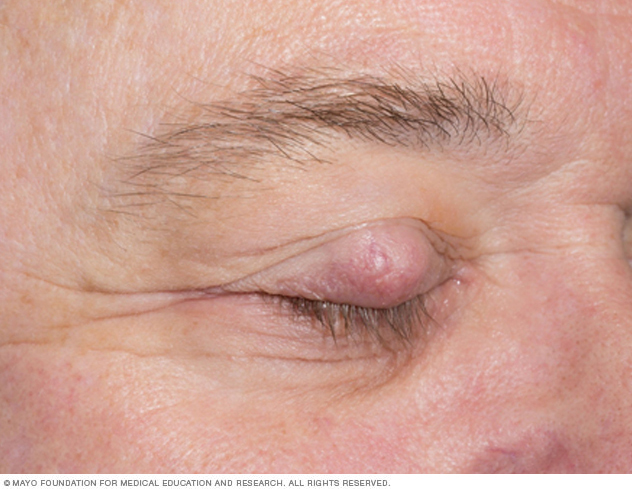

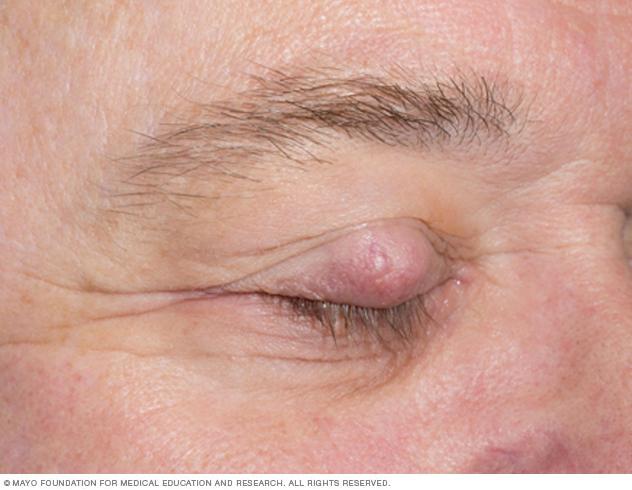

The eyelids contain numerous sebaceous glands (Meibomian glands and glands of Zeis). Because of this, they are the most common site.
Symptoms may resemble:
Chalazion
Recurrent stye
Chronic blepharitis
Eyelid thickening
2. Extraocular Sebaceous Carcinoma


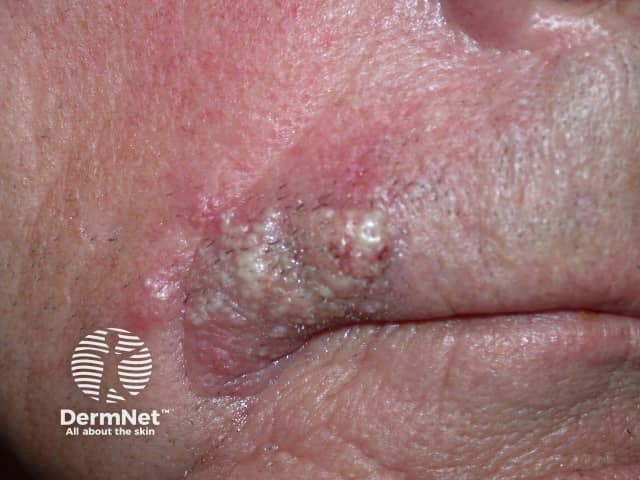
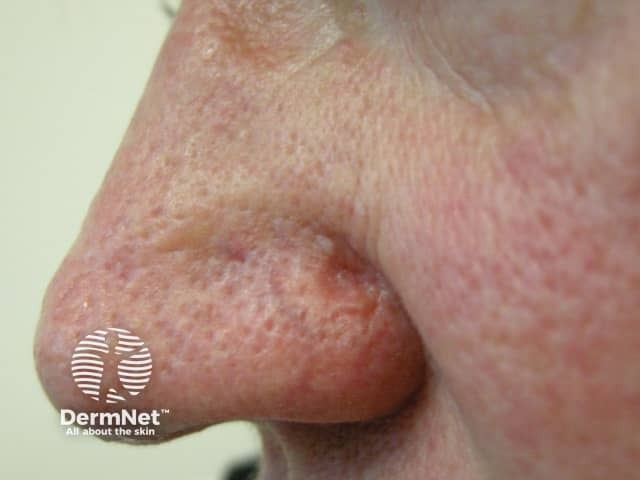
Less commonly, sebaceous carcinoma develops on:
Scalp
Face
Neck
Trunk
Genital area
Extraocular lesions may appear as painless, firm nodules or ulcerated masses.
~Symptoms of Sebaceous Carcinoma
Symptoms vary depending on location.
Ocular Symptoms
Painless eyelid lump
Thickened eyelid
Recurrent chalazion
Loss of eyelashes (madarosis)
Eye irritation or redness
Blurred vision (advanced cases)
Extraocular Symptoms
Firm, yellowish or pink nodule
Slow-growing skin mass
Ulceration
Bleeding lesion
Non-healing sore
Because it can mimic benign conditions, any persistent eyelid or skin lesion lasting more than 4–6 weeks should be evaluated.
~Causes of Sebaceous Carcinoma
The exact cause is not fully understood, but several factors increase risk.
1. Genetic Mutations
Sebaceous carcinoma may be associated with DNA mismatch repair defects.
2. Muir-Torre Syndrome
Muir-Torre syndrome is a rare inherited condition linked to sebaceous tumors and internal malignancies such as colorectal cancer. It is a subtype of Lynch syndrome.
Patients with sebaceous carcinoma — especially younger individuals — may be screened for this syndrome.
3. Radiation Exposure
Prior radiation therapy to the head and neck region increases risk.
4. Immunosuppression
Organ transplant recipients
HIV/AIDS patients
Long-term immunosuppressive therapy
5. Advanced Age
Most cases occur in individuals over 60 years old.
~Risk Factors
Age above 60
Female gender (slightly higher risk in ocular cases)
Asian ethnicity (higher incidence in eyelid cases)
History of radiation therapy
Genetic syndromes (e.g., Muir-Torre syndrome)
Weakened immune system
~How Is Sebaceous Carcinoma Diagnosed?
Early diagnosis is critical.
1. Clinical Examination
Doctors evaluate suspicious lesions that do not respond to standard treatment.
2. Biopsy
A tissue sample is taken and examined under a microscope.
Types of biopsy:
Incisional biopsy
Excisional biopsy
Punch biopsy
3. Histopathology Findings
Under the microscope, sebaceous carcinoma shows:
Irregular lobules of tumor cells
Cytoplasmic vacuoles (lipid droplets)
High mitotic activity
4. Immunohistochemistry
Special stains help differentiate sebaceous carcinoma from other cancers.
5. Imaging Tests
For advanced disease:
CT scan
MRI
PET scan
These help detect spread to lymph nodes or distant organs.
~Staging of Sebaceous Carcinoma
Staging depends on:
Tumor size
Local invasion
Lymph node involvement
Distant metastasis
Advanced cases may spread to:
Regional lymph nodes
Lungs
Liver
Brain (rare)
~Treatment Options for Sebaceous Carcinoma
Treatment depends on tumor size, location, and spread.
1. Surgery (Primary Treatment)
Surgical removal is the gold standard.
Wide Local Excision
Removes tumor with margin of healthy tissue.
Mohs Micrographic Surgery
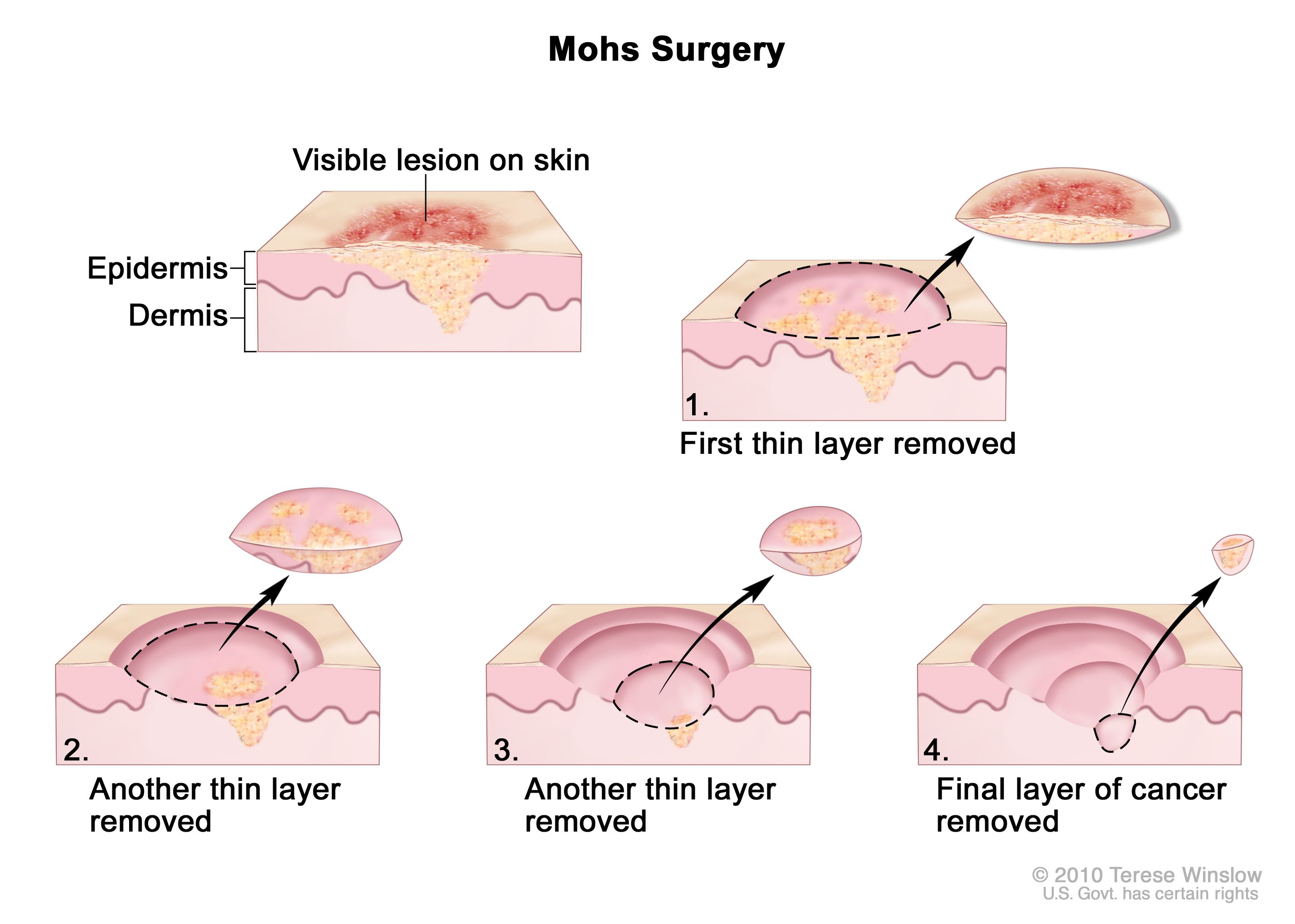


Mohs surgery removes cancer layer by layer while preserving healthy tissue. It has high cure rates and is often used for facial lesions.
2. Sentinel Lymph Node Biopsy
Used if cancer is aggressive or large to check lymph node involvement.
3. Radiation Therapy
Used when:
Surgery is not possible
Margins are positive
Tumor recurs
4. Chemotherapy
Used in advanced or metastatic cases.
Drugs may include:
Platinum-based chemotherapy
5-fluorouracil
Taxanes
5. Immunotherapy
Emerging treatments include immune checkpoint inhibitors for advanced disease.
~Recurrence of Sebaceous Carcinoma
Sebaceous carcinoma has a significant recurrence rate, especially ocular tumors.
Recurrence risk factors:
Delayed diagnosis
Incomplete excision
Lymphovascular invasion
Patients require long-term follow-up for at least 5 years.
~Metastasis and Spread
Sebaceous carcinoma can spread locally and distantly.
Common metastatic sites:
Regional lymph nodes
Parotid gland
Lungs
Liver
Ocular tumors have a higher risk of spreading.
~Survival Rate and Prognosis
Prognosis depends on stage at diagnosis.
Localized disease: 5-year survival rate 78–92%
With lymph node involvement: Lower survival rate
Distant metastasis: Poor prognosis
Early detection significantly improves survival.
~Differential Diagnosis
Sebaceous carcinoma may be confused with:
Basal cell carcinoma
Squamous cell carcinoma
Chalazion
Blepharitis
Merkel cell carcinoma
Accurate biopsy is essential.
~Prevention and Early Detection
There is no guaranteed way to prevent sebaceous carcinoma, but risk can be reduced.
Prevention Tips
Regular skin checks
Avoid excessive radiation exposure
Protect skin from UV radiation
Monitor persistent eyelid lumps
High-Risk Individuals
People with Muir-Torre syndrome should undergo:
Regular dermatologic exams
Colonoscopy screenings
Genetic counseling
~When to See a Doctor
Seek medical attention if you notice:
A persistent eyelid lump
Recurrent chalazion
Non-healing skin lesion
Rapidly growing skin nodule
Loss of eyelashes with eyelid swelling
Early biopsy saves lives.
~Living With Sebaceous Carcinoma
Diagnosis can be emotionally overwhelming.
Patients may require:
Multidisciplinary care (dermatology, oncology, ophthalmology)
Reconstructive surgery (especially eyelid cases)
Psychological support
Support groups and counseling may help patients cope with cancer treatment.
~Frequently Asked Questions (FAQs)
Is sebaceous carcinoma deadly?
Yes, it can be life-threatening if untreated or diagnosed late.
Is it common?
No, it is rare compared to other skin cancers.
Can it recur?
Yes, recurrence rates are significant, especially in ocular cases.
Is it hereditary?
It may be hereditary in cases linked to Muir-Torre syndrome.
~Key Takeaways
Sebaceous carcinoma is a rare, aggressive skin cancer.
Most commonly affects the eyelids.
Often misdiagnosed as a benign lesion.
Early biopsy and surgery improve survival.
Associated with Muir-Torre syndrome.
Long-term follow-up is essential.
~Conclusion
Sebaceous carcinoma is a rare but serious malignancy of the sebaceous glands. Because it frequently mimics benign conditions, early diagnosis requires a high index of suspicion. Surgical excision remains the cornerstone of treatment, and long-term monitoring is critical due to recurrence risk.
If you notice a persistent eyelid lump or suspicious skin lesion that does not resolve, seek immediate medical evaluation. Early intervention significantly increases survival and reduces complications.
Awareness, timely biopsy, and proper oncologic care can make a life-saving difference.




No comments:
Post a Comment